For a Rare Disorder, Is Language Complicating Care?
On the desk of Jesse Keller’s office sits a big red bag about the size of a full sack of groceries, marked “biohazard.” It’s packed with prescription pill bottles filled with fibers, and his desk drawer holds even more of them — along with boxes of specimens in glass slides and a jar filled with a murky unknown liquid. Around the room are other stashes of samples and photographs of skin lesions.
Keller, a dermatologist at Oregon Health and Science University, explains that the items came from patients who have a rare skin condition known as Morgellons disease, marked by experiences of intense, incessant sensations of itch, crawling and burning across the skin, and painful open sores. About a quarter of his patients have the condition, he says, but they are the ones who reach out for help most frequently, as their illness is associated with a lot of anxiety.
He first met people with the disorder in 2016, shortly after he began working at OHSU. The symptoms they described were “unlike anything I had ever heard of before,” he recalled. Morgellons patients typically believe their condition is caused by an infection of fiber-like parasites beneath the surface of the skin. For years, Keller’s patients have been collecting fiber samples and sending them to his office in the hopes they’ll lead him to an explanation of their condition.


But most clinicians consider Morgellons disease a psychiatric condition, known in medical parlance as a delusional infestation or delusional parasitosis. The infection isn’t real, they say, but patients who believe it is may self-inflict real sores and lesions in an effort to excoriate the parasites. Tests typically reveal the perceived invaders to be lint, pet hairs, or carpet fibers that may have glommed onto open, oozing sores. Patients’ fixation on collecting these samples has, itself, come to be seen as a sign of delusional infestation.
There is a disconnect, however, between the way clinicians use the term delusion, and the way many patients perceive it. To psychiatrists, delusional disorders are very real, legitimate medical conditions — ones that cause deep distress to patients and that are often best treated with a low dose of antipsychotic pills. Studies suggest delusional infestation could impact thousands, if not tens of thousands, of Americans annually. To many patients, however, the word “delusional” carries a derogatory meaning; it’s less a diagnosis than an insult. It can therefore be challenging to convince them to accept a medication that suggests their disorder primarily resides in the brain, not the body.
The disconnect has led some patients to turn to alternative treatments offered by a small cadre of clinicians and researchers who see Morgellons as a tick-borne infection associated with infectious agents, including Lyme disease. Proponents of that theory estimate that Morgellons arises in approximately 6 percent of all cases of Lyme disease. But other experts worry that those alternative diagnoses reinforce patients’ beliefs about the origins of their symptoms and delay effective treatment.
The clash over Morgellons has taken a toll on doctors, too. In a letter to the editor published in 2018 in the Journal of the European Academy of Dermatology and Venereology, three quarters of physicians reported feeling stressed when treating patients with delusional infestation. More than a third reported being accused of misdiagnosis and/or wrong diagnostic tests by patients, and some — including Keller — have described being harassed by patients who felt unheard or unseen in their distress. Matthew Grant, an infectious diseases specialist at Yale Medicine, asked in a 2019 editorial whether care for patients of Morgellons or delusional infestation had gotten to the point where “both the provider and the patient are predictably harmed by interacting with one another.”
Keller and others have come to see a need to destigmatize the disorder — and maybe even retire the term delusion altogether. “Patients feel dismissed and unheard when they go to their doctor and are told that they don’t have anything in their skin, and they feel like they’re being told it’s all in their head,” Keller said.
To many patients, however, the word “delusional” carries a derogatory meaning; it’s less a diagnosis than an insult.
One way forward, he believes, is to better understand the disorder’s biological basis, by homing in on nerve signals in the skin and in the brain that might play a part in producing people’s symptoms. The hope is that revealing the condition’s mechanistic roots could lead to better treatments, specifically medications that could improve or cure the disorder.
Meanwhile, the rift over Morgellons, like other medical controversies before it, is pushing some researchers to more closely examine the language of medicine and the ways people perceive it. Health care providers using stigmatizing clinical terms have been found to worsen the care of people with sickle cell disease, substance use disorders, and other conditions. Although psychiatrists may not stigmatize delusions, the word is colloquially used as a synonym for “crazy” or “not objective,” said Kimberly Emmons, a medical rhetoric researcher at Case Western Reserve University. That can be belittling and shape how doctors and patients interact. “Both the doctor and the patient are using the same word,” she said, but “they are not having the same conversation.”
The rise of Morgellons over the past two decades can largely be traced back to a single person, Mary Leitao. In 2001, Leitao was desperate to understand a strange rash on her child’s face, and she refused to believe doctors who said the fibers she observed there were not related to the rash itself. Leitao scoured the internet’s archives of scientific research and found a nearly 400-year-old condition called Morgellons disease that described “harsh Hairs” that broke out on children’s backs. The emergence of these hairs correlated with an easing of cough and convulsions. She adopted the name and set up a website to connect with others experiencing similar symptoms. By early 2009, more than 13,000 families were registered with the website, which was named the Morgellons Research Foundation.
The foundation’s advocacy caught the attention of politicians who urged the Centers for Disease Control and Prevention to further investigate. In 2008, the CDC announced it was launching a study of the illness.
The study, published in 2012, analyzed fibers, skin samples, blood, and urine from subsets of participants. Chemical analysis of fiber samples revealed them to be superficial skin, cotton, or other textiles. And more than three fourths of the participants said their symptoms began in or after 2002, when Morgellons disease first began to surface online. (Researchers have described Morgellons disease as an “meme,” citing the internet as a major contributor to the spread of the term.)
“Both the doctor and the patient are using the same word,” Kimberly Emmons said, but “they are not having the same conversation.”
The authors of the 2012 study concluded that they could not be certain if Morgellons was a new condition or a form of delusional infestation, a disorder with many similar symptoms. Not many clinicians have conducted systematic research on Morgellons since then, said Steven Feldman, a professor of dermatology at Wake Forest University of School of Medicine. And the research that has been done, Keller added, has mostly been led by the Charles E. Holman Morgellons Disease Foundation and motivated by a desire to “prove the infectious trigger.”
One researcher pursuing that line of inquiry is San Francisco-based Raphael B. Stricker, who says he first began to treat tick-borne diseases in the 1990s. Stricker was dismissed from the University of California, San Francisco in 1990 for falsifying data featured in a study on AIDS. (Stricker denies any wrongdoing.) But he has continued to work out of his own private practice in San Francisco.

Researcher Raphael B. Stricker sees Morgellons disease as a skin manifestation generally from tick-borne bacterial infections, and treats it as such.
Visual: Courtesy of Raphael B. Stricker
Stricker sees Morgellons disease as a skin manifestation generally from tick-borne bacterial infections, and treats it as such, using extended courses of the anti-parasitic medication ivermectin, along with combination antibiotics. The duration of time patients need to use these drugs depends on several factors, including how long the infection has been present, he said. Part of the reason he denies the condition is a delusion is because his patients are often professionals including teachers, nurses, and lawyers — “totally normal people,” as he describes them.
Melissa Fesler, a 2023 graduate of UCSF’s doctorate in nursing program and one of Stricker’s long-time collaborators, shares that view. She thinks quality care must begin with changing the beliefs of clinicians who consider Morgellons to be a psychiatric condition — which she imagines could be especially difficult for specialists who have been practicing for decades. “I think it’s really hard to kind of go back and say, “Wow, I’ve been wrong,” or “I have published papers, and they are wrong, and I have failed patients,” Fesler said.
Fesler recalls being introduced to Morgellons disease by Stricker in 2014, about two months after she started working in his private practice. From the start, she says, she “never once doubted that this wasn’t an infectious etiology.”
With microbiologist Marianne Middelveen, Stricker has published several scientific studies supporting this idea. But that body of work has been greeted with skepticism. The datasets the group has presented as evidence of infectious organisms lack the precision needed to confirm the findings, Feldman says.
In a 2021 systematic review, Feldman and his colleagues highlighted that the majority of studies published from January 2010 to April 2021 supporting infectious origins of Morgellons were authored by the same few researchers — a team including Middelveen and Stricker — and that much of their data came from repeatedly studying the same small group of patients with a known intersection of Morgellons and exposure to bacteria causing Lyme disease. “Improper research techniques” and the “selective suppression of contradictory data” can’t be ruled out when interpreting these studies, Feldman and his co-authors wrote in their review. The review also noted that no independent researchers have replicated the team’s findings.

Nevertheless, Stricker and his colleagues’ body of work has been taken seriously by some people. Among them is 83-year-old Carolyn Kolb.
About five years ago, Kolb’s daughter-in-law and grandson visited her at her home in Salem, Oregon. They had been staying with her for less than two days when the family discovered the grandson had lice. They looked up lice centers and went in for treatment. “They didn’t find it on me, but I kept itching,” Kolb says. “I felt like I had them.”
Kolb believes her dermatologist prescribed ketoconazole shampoo, along with either ivermectin or an antibiotic, but she also recalls that the doctor “just kind of blew me off really fast.” The itching persisted and became so severe she would get out of bed at night for a shower to ease the discomfort. Then she noticed she was combing cocoon-like structures out of her hair. Kolb also searched the internet for more information.
She found a book by nurse practitioner Ginger Savely titled “Morgellons: The legitimization of a disease” — a book that embraced the infectious origin view of Morgellons. “It was a complete picture of exactly what I was finding in my brush,” Kolb said. “Then I was pretty sure that this is what I had.”
Psychiatrists define delusions as fixed, false beliefs. But the “delusion” in delusional infestation refers to patients’ beliefs about the cause of their illness, not the reality of their distress or pain. “We know the symptoms are real,” said Peter Lepping, a psychiatrist in the National Health Service system in the United Kingdom. “Sometimes where we disagree is what the origin of the symptoms is, so what the underlying illness is.”
Lepping typically meets patients at a monthly clinic at the Liverpool School of Tropical Medicine that he co-runs with infectious disease specialist Bertie Squire. When presented with a new patient, the clinic first runs various labs and tests to identify possible sources of infection and also conducts psychiatric evaluations. Only once in the last 14 years since the clinic opened have they identified a parasite causing a patient’s illness, Lepping said.
In 2024, Peter Lepping and co-authors published a study that found an antipsychotic drug named amisulpride to be the most effective treatment.
They’re careful to avoid labeling people delusional unless asked directly by the patient. Still, their patients often resist antipsychotic medication, as it implies the condition is somehow false. Lepping said he and his colleagues can typically persuade about half their patients to accept medication. People often struggle with diagnoses of delusions, studies suggest, and tend to consult with numerous doctors to find one who will support their beliefs. One study found patients diagnosed with primary delusional parasitosis saw an average of six physicians before eventually going to a clinic or the emergency room for help.
In 2009, Lepping and another researcher published a review of the literature on delusional infestations. They categorized Morgellons as a variation of the condition; each variation was defined based on what a person believes is causing their symptoms. Worms, mites, and flies were all commonly perceived causes of the skin sores and irritations.
Delusional infestations are unusual in that they can often start suddenly in people who don’t have a history of mental illness. They have also been found to be associated with dozens of potential triggers, including vitamin deficiencies, reactions to antibiotics such as clarithromycin, and stimulant drugs used to treat Parkinson’s disease, ADHD, and other conditions. Morgellons, in particular, is most common in older adults who are otherwise mentally healthy, especially women.
In 2024, Lepping and co-authors published a study that found an antipsychotic drug named amisulpride to be the most effective treatment. Another effective antipsychotic they identified was risperidone. In the U.S., clinicians prescribe pimozide, an antipsychotic like amisulpride that was not included in the study. (Amisulpride tablets are not available in the U.S. but pimozide is.)
Although Lepping said delusional infestation is “a rare illness,” he suggests it’s common enough that there needs to be greater awareness of how to diagnose and treat it. “When you look at the research, most dermatologists will see people with delusional infestation at some point in their career.”
He thinks researchers who continue to classify and treat Morgellons as an infectious disease are genuinely trying to help patients, not mislead or exploit them. Nonetheless, he believes that addressing the condition as an infection — despite evidence to the contrary — hurts patients by delaying access to antipsychotic drugs and other evidence-backed care. “They actively deny them successful and meaningful treatment,” Lepping said. “I think that does cause harm.”
In his clinic, Keller has avoided picking a side on the possible causes of Morgellons. “It could take several decades to really pin down what is the trigger for this,” he said. “In the meantime, I’ve got hundreds of patients who are coming to me desperate for relief.”
In a 2024 research article, Keller and his co-authors found that people with Morgellons reported experiencing a lower quality of life and worse sleep quality than people with other chronic skin conditions such as psoriasis and eczema. The greatest challenge, he says, is the mistrust of health care providers and health care in general.
When patients press Keller to identify the organism or infection responsible for their illness, “I tell them, we might both be dead by the time that happens,” he said. Instead, he steers the discussion to treatment. “How can we get you your life back?”
“It could take several decades to really pin down what is the trigger for this. In the meantime, I’ve got hundreds of patients who are coming to me desperate for relief.”
Carolyn Kolb found her way to Keller through an online search. He prescribed doxycycline to treat the skin lesions, together with gabapentin, a drug that is used off-label to relieve chronic itch, especially when it’s related to nerve pain. The drug combination relieved her symptoms somewhat, and she can sleep through the night again.
Another patient of Keller’s, 32-year-old Rachel Pawelczyk, found him after bouncing from one clinic to another — sometimes traveling thousands of miles from her Connecticut home — and struggling with what she heard. She felt dismissed by some of the providers she saw. “My internist told me it’s a psychiatric condition,” she said. “He doesn’t believe in it.” Eventually, she traveled to Portland to meet with Keller and began a regimen of drugs that aim to improve nerve function and reduce pain and itch, including pregabalin, naltrexone, and a low dose of pimozide.

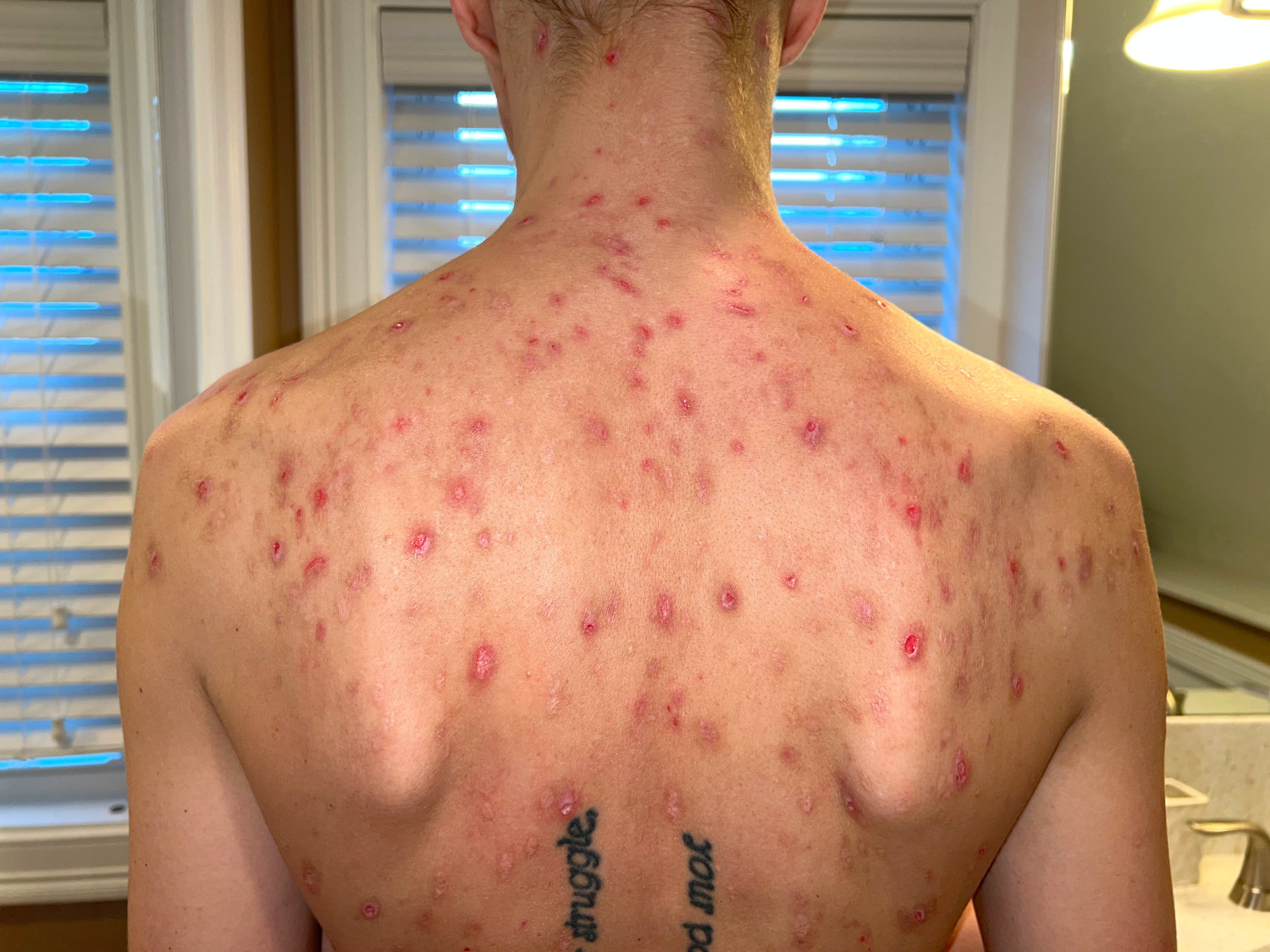
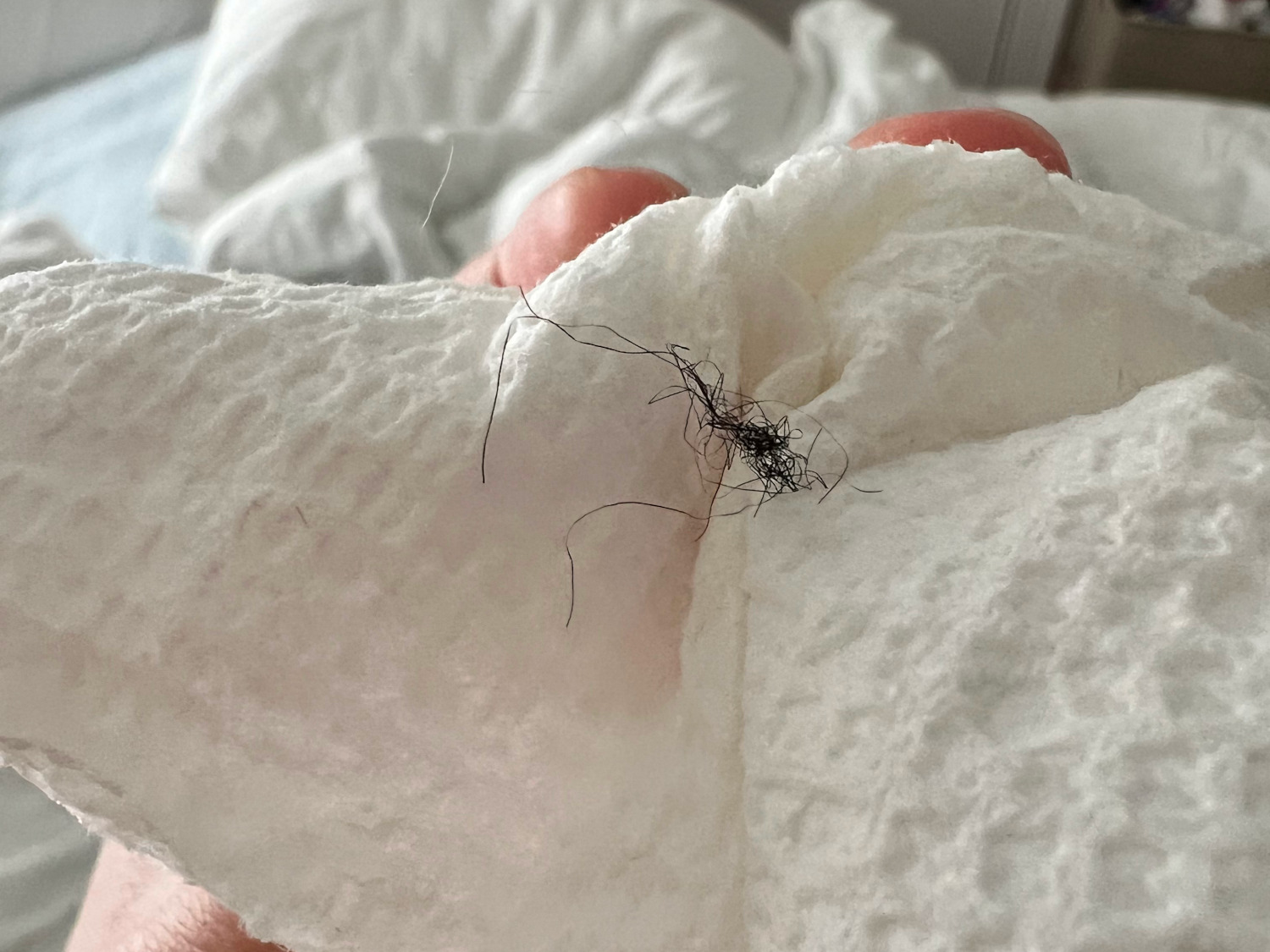
A third patient, Elizabeth, started to notice symptoms in 2018, the summer after a series of treatments for two infections she may have picked up while backpacking. (Elizabeth asked that only her middle name be used in this story, out of concern that details of her condition could harm her employment prospects.) As sores spread over her face, arms, back, and neck, they began affecting her life. Her housemate didn’t want to share a bathroom, worried about contracting whatever was causing Elizabeth’s skin issues. She also started noticing fibers on the open wounds and thought they might be somehow related to her skin problems. She collected the fibers in a plastic bag to show her doctor. She remembers incessant crawling and burning sensations on her skin. “It also felt like someone had a hot knife and was scraping my skin off with it — like how you’d filet a fish,” she said. “It felt like that and I was in a lot of pain.”
The symptoms forced her to drop out of school when she was less than two quarters away from completing her training to be a nurse practitioner. Unable to keep up with her bills, she found herself subsisting on SNAP benefits and living in her house with the utilities turned off. She had started to think her problems were somehow related to her 100-year-old hardwood floors. She steamed the finish off them, then covered them with a chalky insecticide. “My family was worried that I was losing my mind,” she said. “And to be honest, I really was.”
At her early appointments, Keller worked with Elizabeth and her psychiatric mental health nurse practitioner to stop Wellbutrin and her prescription Adderall, the latter of which she had taken for years for her attention-deficit/hyperactivity disorder, or ADHD. (Her provider had increased her dosage to cope with the pressures of her final year of graduate school — the same year that her symptoms began.) Stopping the two medications, she said, was a “big step in the right direction.”
The association between Adderall and Morgellons aligns with one idea about the biochemical origins of a disorder that has, to now, been incredibly difficult to pin down.
Stimulant drugs such as Adderall act to increase levels of the neurotransmitter dopamine. Researchers studying delusions — both delusions of infestation and other kinds — are learning that dysregulated dopamine signals might play a key role in influencing people to believe things that aren’t true.
Dopamine signals are key to processing sensory information in the brain, and MRI scans suggest that errors in dopamine signaling might cause people to misinterpret those cues. When the wind brushes a strand of a person’s hair across their skin, for example, their brain might interpret the sensation as a bug crawling under their skin, Keller says. Drugs that alter dopamine transmission — such as stimulant medications for ADHD and Parkinson’s — could therefore trigger delusional infestations in some people.
“It also felt like someone had a hot knife and was scraping my skin off with it — like how you’d filet a fish. It felt like that and I was in a lot of pain.”
Physical changes in the brain might also be important, especially in older adults. In one recent study, researchers found that the distribution of white matter lesions in older adults’ brains were linked to the sort of delusions they experienced. Of the participants with delusion disorders, around half of the study participants had delusions of infestation, the rest held delusions of persecution or other beliefs unrelated to physical sensations. Those with delusional infestation had more lesions in parts of the brain that help process physical sensations such as touch, and parts that determine how much attention we pay to these sensations. The changes could mean that people with delusional infestations feel things more strongly and are also more prone to assigning unlikely explanations to those sensations, said Robert Christian Wolf, a professor in the Department of General Psychiatry at Heidelberg University, who led the new study. The lesions “explain a mechanism of disrupted belief formation,” he said.
The results primarily apply to older adults, Wolf said, whereas errors in dopamine signaling may be more significant in younger people. The data only provide one possible mechanism of delusional infestation, which is an endpoint of multiple biological pathways that take years to develop, he said. Still, using MRI or brain imaging in the diagnosis of delusional disorders could eventually lead clinicians and patients to effective treatments more quickly. Delusions and hallucinations, Wolf added, “are ultimately consequences of brain changes.”
Emmons, the medical rhetoric researcher at Case Western Reserve University, suggested that understanding the biological mechanisms of mental health conditions can reduce the stigma associated with a diagnosis such as delusion. Emmons sees parallels between the language of delusional disorders and that of depression, the primary focus of her research. Describing clinical depression in terms of brain chemistry “made it more acceptable to prescribe antidepressant medication,” she said, citing selective serotonin reuptake inhibitors, or SSRIs, as one example. “That’s sort of mechanical, right? The mechanical response to a mechanical problem is, you know, you put oil in your car, you put SSRIs in your brain.”
Advocates for more inclusive language have fought to disentangle words for intellectual disability or homosexuality from being used in derogatory ways. But the term “delusion” has been slow to shed its stigma: It is not uncommon to see news headlines that equate being delusional to being uninformed, misguided, or unreal. In his editorial, Grant, the infectious diseases specialist, argued that a diagnosis that included the word delusional “compounds the patients’ suffering,” and suggested that a “first step toward mitigating the very real potential for harm” would be to rename the condition. (Lepping and others say that attempts to rename the condition have failed because patients can use the internet to connect the dots between the alternative names, such as Ekbom syndrome, and delusions.)
Given how deeply entrenched the word is in popular parlance, it may be that the scientific community will need to find another term to describe the condition, Emmons said. In his grand rounds talks, Keller uses the term “dopamine-overload parasitosis,” though he said he has yet to see that phrasing adopted anywhere else.
By June 2023, Elizabeth’s symptoms had subsided significantly. She began working full time as a registered nurse for a care team that works with patients who have psychosis, schizophrenia, and other mental illnesses. She found it satisfying to help people cope with the discrimination and overall toll of these disorders. “I can relate to that from my Morgellons experience,” she said. (Elizabeth has since taken a new job working with a different patient population.)
At OHSU, Keller has been lightly probing the origins of Morgellons, studying, for instance, whether nerve injuries or inflammatory proteins in the skin may play a part in triggering the disorder. But he says his main research focus is on treating symptoms and improving patients’ quality of life.

Even that work makes him feel like a bit of an outlier, he says. A 2025 literature review found that there have been no randomized controlled trials evaluating treatments for Morgellons, nor a concerted effort to develop guidelines for patient care. Despite decades of patient histories and an international community of people who have the disorder there isn’t a cohesive research community for him to lean on.
“I feel like I’m a little bit on an island trying to chip away at this,” he said, “trying to represent my patients the best that I can.”















This is an amazingggg article, wowwww
Wow clearly you are not experiencing any of the things I am. I had a normal life 61 days ago and now I don’t even recognize myself. I find your article very biased and not very knowledge. Perhaps you need to reach out to people who are actually living a nightmareor or hell but I’m going through. I compare this to a Hollywood style of hunger games where nobody acknowledges the hell you are going through… Medical Science doesn’t understand it so therefore they can’t acknowledge it and send me home tell me I’m crazy? I can understand why so many people going through this have such a high suicide rate…. I can’t believe our medical system will not acknowledge this or even do test to try to understand this…
“Fibers were mostly cellulose, consistent with cotton.” Not ‘confirmed as cotton.’ Not ‘matched to commercial textile database.’
Not ‘identical to.’ And ‘Consistent with’ is not a positive ID. Cellulose and cotton-origin cellulose have overlapping but distinguishable IR spectra; engineered nanocellulose has different crystallinity peaks. The study doesn’t mention testing for crystallinity index, degree of polymerization, or nanostructure, all of which would distinguish engineered cellulose from cotton They looked at 23 samples under a microscope and said: Eh, probably cotton.
’Clinical, Epidemiologic, Histopathologic and Molecular Features of an Unexplained Dermopathy.’
UNEXPLAINED.
The title admits they don’t know what it is.
But the conclusion says:
‘No common underlying medical condition or infectious source was identified… shares features with delusional infestation.’
‘Shares features with.’
Not ‘is.’
Not ‘confirmed as.’
‘Shares features with.’
You know what else ‘shares features with’ delusional infestation?
Actual parasitic infections.
Actual environmental exposures.
Actual dermatological conditions that cause itching and lesions.
‘Shares features with’ is meaningless.
But the headlines say:
‘CDC: Morgellons Is Psychiatric’
‘Study Finds No Infectious Cause’
‘Mysterious Condition Called Delusional’
And 15 years later, same half-baked “science.” Fixed beliefs indeed.
I am leaving my comment in the form of a podcast episode, or as I like to call it an audio rebuke with pizazz.
The problem isn’t the language — it’s what the label does. When a diagnosis functions as a stop sign rather than a starting point, it ends the diagnostic process before root cause is understood or a treatment path is established. That’s not medicine; that’s case closure.
The suffering is real. Fine. But real suffering of unknown etiology deserves investigation, not medication-driven sedation and cognitive blunting that precludes further inquiry. Dismissing a patient from the testing and discovery process while simultaneously pathologizing their insistence on answers is gaslighting — and it causes measurable harm.
The stimulant angle doesn’t hold up. Four-year-olds get this condition. No child that age is a stimulant over-user. If the hypothesis can’t survive that one data point, it isn’t a root cause; it’s a correlation being dressed up as explanation.
Finally: it is neither ethical nor within the scope of dermatological competency to prescribe powerful psychotropic medications without a mental health professional running point. That’s a boundary of professional scope, not opinion.
Stop being so rational Kate. We’re supposed to be nutjobs, and you’re making way too much sense.
OSU recently replicated the Middelveen findings. https://scholars.okstate.edu/en/publications/molecular-analysis-of-the-systemic-dermatoses-of-morgellons-disea/